|
Features:
Grizzly
bear | He's
cooking

Medicine
men
For a
thousand years, South American healers have enlisted a certain weed to
cure coughs, colds, even tuberculosis. Now, a small group of researchers
-- led by UC-Irvine Associate Prof. Edward Robinson Jr. '84 and TCU Chemistry
Prof. Manfred Reinecke -- believe that something in wira wira may help
defeat the virus that causes AIDS.
By
Nancy Bartosek

 IT
TOOK a thousand lifetimes of knowledge to build the cramped biohazard
level II lab at UC-Irvine, a sterile environment where blue antibacterial
lights bathe stainless steel countertops and workers wear protective covers
when entering the restricted space. IT
TOOK a thousand lifetimes of knowledge to build the cramped biohazard
level II lab at UC-Irvine, a sterile environment where blue antibacterial
lights bathe stainless steel countertops and workers wear protective covers
when entering the restricted space.
The small
room, cluttered with plastic bottles and boxes and specialized equipment,
is often unoccupied, the only sound a constant rush of air sucked through
high-tech filters. But that doesn't mean nothing is going on.
In a red
liquid incubating in a thick steel cabinet labeled BIOHAZARD, a microscopic
war is being waged. It is a carefully contrived battle that may defeat
a deadly killer. Dr. W. Edward Robinson Jr. '84, PhD, (above) heads the
research team lining up the petri dish scrimmages between the virus that
causes AIDS and a compound that stops the progression of the disease --
a substance they discovered. It is slow and tedious work performed by
few on a limited budget.
If they
unlock the secrets in the red solution, millions of people infected with
HIV may live longer, healthier lives.
Like most
scientific breakthroughs, the discovery has brought national attention
to Robinson and company.
There is
acclaim.
There is
criticism.
And there
is the youthful Robinson with the same smile and response to both: "It
works."
EVERY DAY, Robinson and his assistants don green paper smocks and two
pairs of surgical gloves before venturing through the inner door of Robinson's
primate retrovirology lab. Working methodically at protective, glass-enclosed
hoods, they mix fetal calf serum (which provides important nutrients and
growth factors to the cells), active HIV cells and one of several compounds
they are testing. When the mix is right, HIV infection is stopped.
The stuff
of miracles? Perhaps. But to hear the scientists involved tell it, it's
more a matter of creative thinking, a touch of serendipity and a heap
of persistence. Robinson and TCU Chemistry Prof. Manfred Reinecke stumbled
on the compound's hidden talent in 1989 when the former was studying the
AIDS virus at Vanderbilt University.
Reinecke
was on campus for a conference. Later, over dinner at a Nashville steak
house, he told Robinson about some Bolivian plants he was breaking down
chemically. Reinecke had been thinking to himself, Could Bolivian medicine
men, practicing ancient healing arts for centuries, know something we
don't? Now he was asking Robinson if he would test the compounds for medicinal
uses.
"I wasn't
expecting much, but I thought it would be interesting," Robinson said.
"The bottom line was we got a very high hit rate. Eleven of the first
18 plants looked very promising as leads for anti-HIV activity."
Something
in the compounds Reinecke sent worked against the virus without killing
the host cells the HIV was infecting, something similar drugs weren't
able to do. The next step: figure out what in the compound worked, and
why.
Caffeic
acid derivatives -- the active ingredients in Robinson's and Reinecke's
successful compound -- are nothing new. They can be found in chicory bark,
green coffee beans, and a gangly Andean mountain weed called wira wira.
What wasn't known was that these minuscule molecules have a powerful effect
on an enzyme called integrase, a necessary ingredient in the HIV infection
process of immune cells. It took Robinson and Reinecke five years of testing,
filtering, eliminating and retesting the rich, white powder extracted
from various plants before they could say for certain what inhibited the
growth of HIV. They didn't understand how, they only knew it did. And
that was enough to keep them searching for answers.
IT'S HARD to imagine that one milligram of white dust (imagine the size
of a pencil tip) could have much of an effect on anything. But in Robinson's
lab, that powder packs a wallop.
Which is
probably why the Bolivian medicine men, known by locals as "lords of the
medicine bag," continue to grind up wira wira, the white powder's source,
traversing from the valleys of the Amazon to the tops of Andean peaks,
administering healing herbs since long before Western medicine and HMOs.
At least
that's what Reinecke figured in 1988 as he listened to UT-Arlington ethnobotanist
Joseph Bastien talk about his work with the Kallawaya Indians, an Andean
mountain tribe that has farmed, gathered herbs and perfected their healing
skills for 1,000 years. This small group of medicine men, today numbering
about 350, even practiced successful brain surgery as early as 500 A.D.,
using only locally gathered medicines and handmade tools.
Reinecke's
interest was piqued; he approached Bastien about acquiring some plants
to test for biomedical purposes.
"Why not?"
replied Bastien. Small grants from TCU and the Fort Worth Herb Society
sent Bastien south and some plants north. "We were just a small-potatoes
operation," Bastien recalls.
Several
of the Bolivian plants -- including wira wira and carqueha -- showed strong
antiviral activity from the beginning. But winnowing one pure compound
from a plant containing hundreds, especially when the compound is unknown,
is arduous at best. And expensive.
Initial
results were promising enough for the National Institute of Health to
give Robinson and Reinecke a three-year grant in 1991. Much of that time
was spent finding out where the compounds didn't work.
"They didn't
work at sites that all the other drugs worked at and that were easy to
measure," Robinson said. "Trying to figure out how they worked was a tough
thing. We knew they were antiviral but we didn't know how."
During that
same time, Robinson was finishing his medical degree then moving to UC-Irvine
to establish his own lab. A second NIH grant in 1997 kept them on the
trail. The result? Eleven compounds in the dicaffeoyltartaric and dicaffeoylquinic
acids group inhibited viral replication. L-chicoric acid, their lead compound
(based on the chemical properties in the two acids that had the antiviral
activity), was synthesized in Reinecke's lab.
"We now
have a much better idea why the compounds work against the virus and why
they work against the enzyme integrase," Robinson said. "The goal over
the next several years is to look at the structure of the drugs, what
their activity is and determine how to make better molecules. The hope
is that within the next two or three years we'll have something that's
potent and safe enough to test in animals, then people."
Robinson's
compounds (which he, Reinecke, TCU and UC-Irvine are trying to patent)
not only work, they work better, or synergistically, with existing anti-HIV
drugs. Sort of a turbo-boost effect.
"It's like
quadrupling the effect but only adding twice as much," Robinson said.
Synergy is a critical plus when fighting living organisms. Consider, for
example, man's lack of success obliterating tuberculosis or herpes.
"Nature
finds ways to get around our attempts," Robinson said. "All we're doing
is adding drugs to prevent a bacteria or virus. Kill off 99 percent of
the bugs, and that one percent grows up as the predominant group and is
now immune to the therapy." HIV is tough to treat because every time it
replicates, it mutates. Design a drug for one strain and it changes and
the drug no longer works.
Drug cocktails
containing compounds that attack more than one stage of the disease can
sometimes circumvent that. The idea is that if the virus mutates past
one therapy, it probably won't around two, or three.
"It is clear
there will never again be a single drug treatment for HIV," Robinson said.
"Our drugs must work in the presence of existing anti-HIV agents because
if they don't, they won't ever work. You cannot use a single drug for
HIV therapy."
BAGS OF still-untested Bolivian plants lie patiently in Reinecke's storage
room, waiting for their secrets to be released. With limited funding and
personnel, the process continues at an academic pace.
"At some
point this will have to be taken over by a pharmaceutical company that
can put teams of people and money into the development of a usable drug,"
Reinecke said. Several companies have expressed interest but there haven't
been any takers -- yet. "I think we're still on the edge, teetering,"
Robinson said. "Is it going to fall off the edge because we've got the
best things we can ever get? Are we going to take the leap to the other
side where it's in people? I don't know yet."
The likelihood
of developing a new drug is very small. Robinson's work is still at stage
one: developing a compound that works in tissue culture. Only about one
percent of those drugs ever make it into people because many of them fall
out at animal trial stage. If they do go into people, an equal number
are too toxic or don't work well enough or the mutations come so fast
you can't keep up.
"Those things
are hurdles along the way," he said. "We're still working over the first
hurdle now."
Robinson
is more optimistic than that statement sounds. His tests have repeatedly
proven effective, and each step has given them more reason to forge ahead.
"We feel very confident that the drugs work," Robinson said. "We sent
them out blinded and they were identified as functional. We have repeated
the data 1,000 times under various permutations over the last five years.
"They always
work."
So, forward
they go. Reinecke, who for 34 years has encouraged and prodded TCU students
who aspire to be doctors, says this work is the most exciting research
of his career. "It's something significant."
The work
isn't just a clinical exercise for Robinson, either.
"As corny
as it sounds and perhaps as unreasonable as it is, I want to make an impact
on the treatment or prevention of HIV," he said. "If I could come up with
a drug that could be used in the Third World because it was cheap enough,
or a drug that would lower side effects and improve life spans, it would
have an impact on hundreds of thousands of people. I could never in my
career as a physician have an impact on that many people. That's why I
do this."
Robinson
pauses, nods and smiles a knowing smile.
"So far
we've had a lot of success. I think this is going to continue to progress."

The drug
war

Tracking
a killer
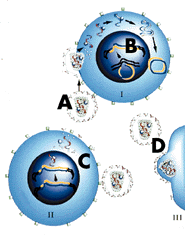
The virus (A) must enter and join with the host cells' chromosome
(B) for infection to take place. After infection, the diseased cell
replicates (C), then sends the virus out (D) to infect still-healthy
immune cells. |
|

When a person
is infected with the human immunodeficiency virus, they become a host
to cells that infect immune cells in three distinct stages, each involving
a separate enzyme. Each step must occur for the virus to live and reproduce
itself.
Currently
drugs are administered in the United States that generally stop or slow
the first and the third interactions, which involve enzymes respectively
called reverse transcriptase and protease. So far no one except UC-Irvine
researcher Dr. W. Edward Robinson '84 has found a drug that will effectively
stop the second stage of cell infection, which involves the enzyme integrase.
The compounds
he and Chemistry Prof. Manfred Reinecke have isolated are effective integrase
inhibitors that work in cell tissue without destroying the host cell.
If research continues to progress positively, these compounds will be
tested in animals within three or four years. In five to seven years there
could be drugs available for human testing.

Contact
Robinson at ewrobins@uci.edu or Reinecke at m.reinecke@tcu.edu.
Top
|



